Anti-Seizure Drugs (Anti-epileptics)
Special Points:
- Phenytoin produces Gingival Hyperplasia and Hypertrophy.
- Sodium Valproate is a broad spectrum antiepileptic.
- Newer BROAD SPECTRUM ANTIEPILEPTICS: Lamotrigin, Topiramate, Zonisamide
- Ethosuximide is specific in inhibiting the T-type calcium channels and is specific to treat absence seizure (Petit Mal Epilepsy).
- Carbamazepine is drug of choice for Trigeminal Neuralgia.
- Phenytoin is known to worsen absence seizure and hence never used for treating absence seizure.
- Lorazepam / Diazepam is drug of choice to stop convulsions.
- Phenytoin, Carbamazepine, and Barbiturates – all are inducers of CYP3A4 system (Hepatic Microsomal Enzyme System – HMES), whereas Valproate is an inhibitor !!
- Contraindication for Barbiturates/Phenobarbitone: Acute Intermittent Porphyria
- Most of the antiepileptic drugs are teratogenic. Phenytoin produces a syndrome called Hydantoin Syndrome – may consist of neural tube defects such as spina bifida, and other structural defects like craniofacial abnormalities or congenital heart defects, as well as growth retardation, and also mental retardation.
- A drug used for long term, on a daily basis, to prevent seizures in a known patient with epilepsy is called an ANTI-EPILEPTIC DRUG; a drug used symptomatically, to stop convulsions (irrespective of the cause of convulsions), is called an ANTI-CONVULSANT.
- Gabapentin, Tiagabine, Pregabalin, and Levetiracetam are mainly useful in partial seizures.
- Anti-epileptic as well anti-arrhythmic: Phenytoin
- Other uses of anti-seizure drugs: -Trigeminal Neuralgia, Other neuropathic pains (multiple sclerosis, diabetic neuropathy, post-herpeitic neuralgia), Bipolar disorder, Also Acute Mania, Migraine.
- Antiseizure/Anticonvulsant drugs used as mood stabilizers in Bipolar Disorder: Carbamazepine, oxcarbazepine, topiramate, gabapentin, Valproate(rapid cycles), lamotrigine (depressive phase)
- Antiseizure drugs useful in Trigeminal Neuralgia and other neuropathic pains: Carbamazepine, Pregabalin, Gabapentin
Seizure: An episode of brain dysfunction due to abnormal electrical discharges of cerebral neurons.
Seizure may be associated WITH or WITHOUT CONVULSIONS.
Sometimes the word “Non-convulsive seizure” may be used to indicate the episode of brain dysfunction (seizure), where there are no convulsions.
SAQ/LAQ/Viva
Mention adverse effects of Phenytoin sodium (Phenytoin) (Dilantin)
Phenytoin has low therapeutic index. Its adverse effects are as follows:
- Gingival Hyperplasia and Hypertrophy, and bleeding gums
- Vestibulo-Cerebellar Syndrome manifesting in the form of ataxia (Incoordination of movements), Vertigo (Sensation of moving around), Nystagmus (Involuntary movement of eyeballs), Dysarthria (Difficulty in articulation for speech), Blurring of vision, ocular pain
- Coarsening / flattening of facial features, hypertrophy of facial subcutaneous tissue, hypertrichosis (Phenytoin facies)
- Hirsutism, Acne
- Delusions, hallucinations, behavioral changes
- Deficiency of Vitamin D, Osteomalacia
- Deficiency of Vitamin B12, folic acid, Vitamin K, Megaloblastic anemia, peripheral neuropathy
- Teratogenic Effects: Fetal Hydantoin Syndrome: CCranio-Facial defects, Heart defects, Hypoplastic phalanges, Microcephaly, Neural tube defects – Spina bifida. and other malformations
- Phenytoin induces hepatic microsomal enzymes and can increase the metabolism and decrease the effect of many drugs including oral contraceptives, doxycycline, theophylline, warfarin and many others.
LAQ/SAQ/Viva
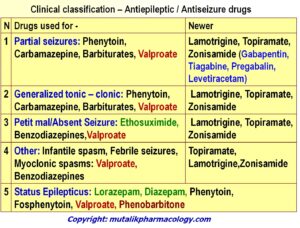
Write clinical classification of Antiepileptic / anticonsulvasant / Antiseizure drugs with examples.
Classification is a way of arranging groups of drugs. The way to classify may have different basis every time.
Clinical classification means the way the drugs are used clinically in various disease states. So here is the clinical classification.
SAQ/LAQ/Viva
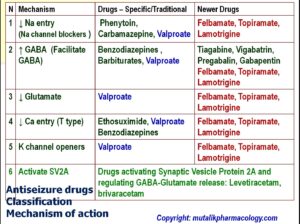
Classify Antiepileptic / Antiseizure drugs based on mechanism of action:
Epilepsy may have some probable mechanisms as follows:
- Increased sodium entry into cells leading to excitation
- Decreased GABA ergic (GABAminergic transmission) (GABA is an inhibitory neurotransmitter – inhibition of its inhibitory effect may lead to excitation)
- Increased Glutamate transmission (Glutamate is an excitatory neurotransmitter – its increase will lead to excitation)
- Increased calcium entry into cells through the T type calcium channels (leading to excitation)
- Blocking of K (potassium) channels (Kv7 channels)
The drugs used in epilepsy may reverse one or more of the above mechanisms. The table below shows the gross / major mechanism of action of various anti-seizure drugs. (Upward arrow stands for increase and downward arrow stands for decrease)